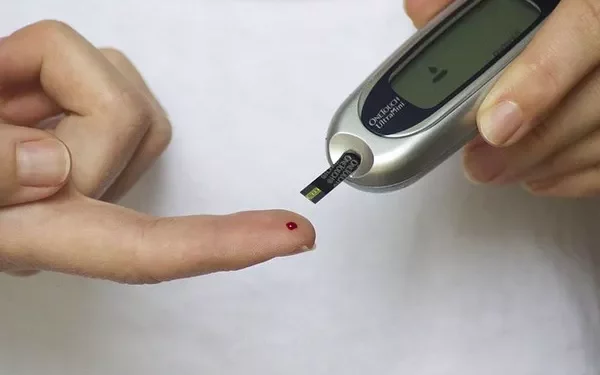
Blood glucose regulation is a fundamental aspect of health, especially for individuals with diabetes. Understanding what influences your glucose levels is essential for managing blood sugar and preventing complications. Blood sugar levels can fluctuate due to a variety of factors, including diet, physical activity, medication, and emotional stress. In this comprehensive article, we will explore the multiple factors that affect blood glucose levels, providing valuable insights into how these variables work together and offering strategies to manage them effectively.
Introduction to Blood Glucose and Its Regulation
Glucose is the primary source of energy for the body’s cells. After we consume food, especially carbohydrates, glucose enters the bloodstream, causing blood sugar levels to rise. In response, the pancreas releases insulin, a hormone that helps transport glucose from the blood into cells for energy or storage.
For individuals without diabetes, the body maintains blood glucose levels within a narrow range. However, for those with diabetes or insulin resistance, this regulation becomes impaired, leading to fluctuations in blood glucose levels. These fluctuations can be either hyperglycemia (high blood sugar) or hypoglycemia (low blood sugar), both of which present health risks.
Understanding the factors that influence blood glucose can empower individuals to take control of their health and make informed decisions regarding diet, lifestyle, and medication management.
Diet: The Most Direct Influencer of Blood Glucose Levels
Diet is one of the most significant factors affecting blood glucose levels. The types of foods you eat, the amount you consume, and the timing of meals can all directly influence how much glucose enters your bloodstream and how quickly it does so.
Carbohydrates and Blood Sugar
Carbohydrates, found in foods such as bread, rice, pasta, fruits, and vegetables, are broken down into glucose during digestion. The amount of carbohydrates you consume plays a crucial role in how much glucose will be available for the body to use.
Simple vs. Complex Carbs: Simple carbohydrates, such as those found in sugary snacks and beverages, are rapidly digested and absorbed, causing a quick spike in blood sugar. On the other hand, complex carbohydrates, found in whole grains, legumes, and vegetables, are digested more slowly, providing a more gradual release of glucose into the bloodstream.
Glycemic Index (GI) and Glycemic Load (GL): The glycemic index is a scale that measures how quickly carbohydrate-containing foods raise blood sugar. Foods with a high GI, such as white bread, cause a rapid increase in blood sugar. Low-GI foods, like sweet potatoes and most fruits, cause a slower, more stable rise. Glycemic load takes both the GI and the portion size into account, offering a more accurate picture of how a food will affect blood glucose levels.
Protein and Fat’s Impact on Glucose
While proteins and fats don’t directly raise blood sugar levels, they can influence how glucose is absorbed. Protein-rich foods, such as meat, eggs, and legumes, can cause a modest increase in blood glucose, but this effect is generally slower and less pronounced than carbohydrates.
Fats, particularly healthy fats from sources like avocados, olive oil, and nuts, can help stabilize blood sugar by slowing down the digestion and absorption of carbohydrates. When consumed in balanced amounts, they can help manage glucose levels and prevent rapid fluctuations.
Portion Sizes and Meal Timing
In addition to the type of food consumed, portion size plays a critical role in how much glucose is absorbed into the bloodstream. Large meals, especially those rich in carbohydrates, can overwhelm the body’s ability to produce insulin, leading to higher blood glucose levels. Eating smaller, more frequent meals can help stabilize glucose levels throughout the day.
The timing of meals also matters. Skipping meals or going too long without eating can lead to low blood sugar levels, especially in individuals taking insulin or medications that lower blood glucose. Conversely, eating too frequently or consuming too many carbohydrates at once can cause spikes in blood sugar.
Alcohol and Blood Glucose
Alcohol has a unique impact on blood glucose levels. Initially, alcohol can cause an increase in blood sugar, particularly when consumed with sugary mixers. However, the liver prioritizes metabolizing alcohol over maintaining normal glucose levels, which can lead to a drop in blood sugar, especially when consumed in excess or on an empty stomach.
For individuals with diabetes, it’s essential to monitor blood glucose levels closely when consuming alcohol. Drinking in moderation, consuming alcohol with food, and choosing low-sugar alcoholic beverages can help manage glucose levels more effectively.
Physical Activity: Exercise and Its Influence on Glucose
Physical activity plays a crucial role in blood glucose management. Regular exercise helps the body use insulin more efficiently and can lower blood glucose levels, making it an essential part of diabetes management.
How Exercise Affects Blood Sugar
Exercise improves insulin sensitivity, meaning the body can use insulin more effectively, allowing glucose to enter cells more efficiently. This can help lower blood glucose levels, particularly for those with insulin resistance. The type, intensity, and duration of exercise can all influence blood sugar.
Aerobic Exercise: Activities such as walking, running, swimming, and cycling help improve cardiovascular health and can lower blood glucose levels by increasing insulin sensitivity.
Strength Training: Resistance exercises, such as weightlifting, can help build muscle mass, which improves the body’s ability to store and use glucose efficiently.
Exercise-Induced Hypoglycemia
While exercise is generally beneficial for blood glucose control, it can also lead to low blood sugar, particularly if someone is on insulin or takes medications that increase insulin secretion. Physical activity can increase the uptake of glucose by muscles, lowering blood glucose levels, and potentially causing hypoglycemia.
To prevent exercise-induced hypoglycemia, individuals should monitor their blood glucose before, during, and after exercise. It may also be necessary to consume a small snack containing carbohydrates before or after exercise to maintain stable blood glucose levels.
The Timing of Exercise and Blood Sugar Control
The timing of exercise can influence how blood sugar is affected. For example, exercising after a meal can help lower postprandial blood glucose levels, while exercising on an empty stomach may lead to lower glucose levels more quickly. Some individuals may need to adjust their medication dosages or meal plans based on their exercise routine to avoid hypoglycemia or hyperglycemia.
Stress: Emotional and Physical Stressors on Blood Glucose
Stress is another significant factor that can impact blood glucose levels. Both emotional and physical stress can lead to temporary increases in blood sugar levels, as the body releases hormones like cortisol and adrenaline in response to stress. These hormones increase blood glucose to provide energy for the “fight or flight” response.
Chronic Stress and Insulin Resistance
Long-term, chronic stress can contribute to insulin resistance, where the body’s cells become less responsive to insulin. This results in higher blood glucose levels, which can be especially problematic for people with diabetes. Stress management techniques, such as mindfulness, relaxation exercises, deep breathing, and regular physical activity, can help mitigate the effects of stress on blood glucose.
Acute Stress and Blood Glucose Spikes
Acute stress, such as a stressful event or illness, can cause a temporary spike in blood glucose levels. It’s not uncommon for people with diabetes to experience elevated blood sugar during periods of emotional or physical stress. Coping mechanisms and lifestyle adjustments, including adequate rest, exercise, and stress-relieving activities, can help minimize the impact of stress on blood glucose.
Medications: Insulin and Other Blood Sugar-Lowering Drugs
Medications are often necessary for managing blood glucose in people with diabetes, but they can also influence glucose levels in various ways. The type and dosage of medication used can significantly affect how blood glucose fluctuates throughout the day.
Insulin Therapy
For individuals with type 1 diabetes or advanced type 2 diabetes, insulin therapy is a cornerstone of treatment. Insulin helps regulate blood glucose by facilitating the transport of glucose from the blood into cells. Different types of insulin (rapid-acting, short-acting, long-acting) work at different rates, and understanding how each type affects blood glucose is essential for avoiding both hyperglycemia and hypoglycemia.
Insulin Sensitivity: People with diabetes may need to adjust their insulin dosages based on factors like diet, exercise, and stress levels. Insulin sensitivity, which refers to how effectively the body responds to insulin, can vary throughout the day and under different conditions.
Oral Medications for Type 2 Diabetes
Medications like metformin, sulfonylureas, and DPP-4 inhibitors are commonly prescribed for type 2 diabetes. These drugs help manage blood glucose by increasing insulin sensitivity, stimulating insulin production, or slowing glucose absorption. The timing of these medications, as well as any changes in dosage, can affect blood glucose levels, and adjustments may be needed based on diet and exercise.
Medication-Induced Hypoglycemia
Certain diabetes medications, particularly sulfonylureas and insulin, can increase the risk of hypoglycemia, especially if meals are skipped or delayed. To prevent low blood sugar, it’s important to closely monitor blood glucose levels and follow the healthcare provider’s instructions on medication timing and dosages.
Illness: How Sickness Can Affect Blood Glucose
Illness, such as a cold, flu, or infection, can cause fluctuations in blood glucose levels. When the body is fighting an infection, stress hormones are released, which can lead to higher blood glucose levels. At the same time, if appetite is reduced due to illness, blood glucose may drop, especially in individuals who are taking insulin or other medications that lower blood sugar.
Fever and Infection
Fever and infections typically raise blood glucose levels as the body’s response to illness increases the production of stress hormones. Managing blood glucose during illness may require adjustments in medication, increased monitoring of glucose levels, and a careful balance of food and hydration.
Dehydration and Blood Glucose
Dehydration, which can occur during illness, can also have a significant impact on blood glucose levels. When the body is dehydrated, glucose can become more concentrated in the blood, leading to higher blood sugar levels. It’s essential to drink plenty of fluids, especially water, to maintain proper hydration during illness.
Conclusion
Blood glucose levels are influenced by a complex interaction of factors, including diet, physical activity, medications, stress, and illness. Understanding these factors and how they affect blood glucose can help individuals with diabetes take proactive steps to manage their condition. By monitoring glucose levels regularly, making informed dietary choices, managing stress, and working closely with healthcare providers, it is possible to maintain optimal blood sugar control and reduce the risk of complications.
Managing blood glucose is a dynamic process, requiring constant attention to daily habits and lifestyle factors. With the right tools and knowledge, individuals with diabetes can achieve a healthy balance, improving both their quality of life and long-term health outcomes.
Related topics: