Understanding when blood glucose levels reach a point where they signal prediabetes is crucial for preventing the progression to type 2 diabetes. Prediabetes, a condition in which blood glucose levels are higher than normal but not yet high enough to be diagnosed as diabetes, is often a silent precursor to more severe health complications. Early detection of prediabetes can lead to lifestyle changes that help delay or even prevent the onset of type 2 diabetes.
The Importance of Blood Glucose Monitoring
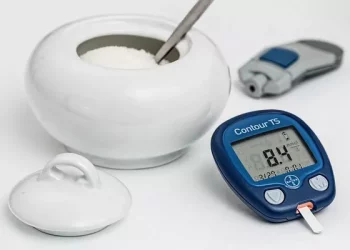
Blood glucose monitoring plays a pivotal role in diagnosing and managing diabetes. Glucose is the primary source of energy for the body’s cells, and its levels in the bloodstream are tightly regulated. When the regulation mechanism is disrupted, such as in prediabetes or diabetes, the body cannot maintain glucose within normal limits, leading to potential health issues.
Monitoring blood glucose levels regularly allows healthcare professionals to detect abnormalities early and take preventive or corrective actions. For individuals concerned about their risk for prediabetes or diabetes, understanding the various blood glucose tests and their corresponding numbers is essential.
What is Considered Pre-Diabetes?
Prediabetes is characterized by blood glucose levels that are elevated but not yet high enough to meet the criteria for a diabetes diagnosis. However, it is a significant warning sign that the body’s insulin regulation mechanisms are under strain. Insulin is a hormone that helps regulate blood sugar levels by facilitating glucose uptake by cells for energy. In prediabetes, the body either becomes resistant to insulin or does not produce enough of it to maintain normal blood sugar levels.
The diagnosis of prediabetes is typically made based on the following tests:
1. Fasting Blood Glucose Test
The fasting blood glucose test measures the level of glucose in the blood after an overnight fast (at least 8 hours without food or drink except water). This test is one of the most commonly used to diagnose prediabetes.
-
Normal: A fasting blood glucose level of less than 100 mg/dL (milligrams per deciliter).
-
Prediabetes: A fasting blood glucose level ranging from 100 to 125 mg/dL.
-
Diabetes: A fasting blood glucose level of 126 mg/dL or higher on two separate occasions.
The prediabetic range of 100-125 mg/dL indicates that the body is starting to have difficulty processing glucose effectively. If fasting blood glucose remains within this range, it is critical to take proactive measures to prevent further progression to diabetes.
2. Oral Glucose Tolerance Test (OGTT)
The oral glucose tolerance test (OGTT) is another diagnostic tool used to assess how the body handles glucose. After an overnight fast, the individual drinks a sugary solution containing 75 grams of glucose, and blood glucose levels are measured at intervals, usually at 2 hours post-drink.
-
Normal: A 2-hour blood glucose level of less than 140 mg/dL.
-
Prediabetes: A 2-hour blood glucose level between 140 and 199 mg/dL.
-
Diabetes: A 2-hour blood glucose level of 200 mg/dL or higher.
The OGTT is particularly useful in diagnosing insulin resistance, which is a hallmark of prediabetes. Insulin resistance occurs when the body’s cells become less responsive to insulin, requiring the pancreas to produce more insulin to achieve the same effect. Over time, this can lead to higher blood glucose levels.
3. Hemoglobin A1c Test
The hemoglobin A1c test measures the average blood glucose levels over the past 2-3 months. This test is often preferred for its convenience since it does not require fasting. It is especially valuable for monitoring long-term blood sugar control and providing insights into trends.
-
Normal: An A1c level of less than 5.7%.
-
Prediabetes: An A1c level between 5.7% and 6.4%.
-
Diabetes: An A1c level of 6.5% or higher.
The A1c test reflects the percentage of hemoglobin in the blood that has glucose attached to it. As blood glucose levels rise, more glucose attaches to hemoglobin, which is reflected in a higher A1c level. An A1c in the prediabetic range suggests that the individual’s average blood glucose levels over the past few months have been elevated but not to the extent that warrants a diabetes diagnosis.
Risk Factors for Prediabetes
Certain risk factors increase the likelihood of developing prediabetes, and understanding these can help individuals take preventive steps. These include:
Age: Individuals aged 45 or older are at increased risk.
Family history: A family history of diabetes can elevate the risk of prediabetes.
Obesity: Excess weight, especially abdominal fat, contributes to insulin resistance.
Inactivity: Lack of physical activity is a major risk factor.
Ethnicity: Certain ethnic groups, including African American, Hispanic, Native American, and Asian American populations, are more likely to develop prediabetes.
Gestational diabetes: Women who developed diabetes during pregnancy (gestational diabetes) are at higher risk of developing prediabetes later in life.
High blood pressure: Blood pressure readings above 140/90 mmHg are linked to an increased risk of prediabetes.
Abnormal cholesterol levels: Low HDL cholesterol or high triglycerides can be indicative of prediabetes.
While these risk factors do not guarantee that an individual will develop prediabetes, they provide valuable information for healthcare professionals in identifying those who may benefit from early screening.
The Silent Nature of Prediabetes
One of the challenges in identifying prediabetes is that it often develops without noticeable symptoms. Many individuals with prediabetes may feel perfectly fine and are unaware that their blood glucose levels are elevated. Without symptoms, it is crucial for individuals at risk to undergo regular screenings, especially if they have any of the aforementioned risk factors.
If left untreated, prediabetes can progress to type 2 diabetes, which is associated with a higher risk of complications such as heart disease, kidney damage, nerve damage, and vision problems. Early detection, however, offers an opportunity to implement lifestyle changes that can help prevent or delay the onset of type 2 diabetes.
Lifestyle Changes to Prevent or Reverse Prediabetes
For individuals diagnosed with prediabetes, making healthy lifestyle changes can significantly reduce the risk of progressing to type 2 diabetes. Key changes include:
1. Weight Loss
Losing even a modest amount of weight—around 5-10% of body weight—can improve insulin sensitivity and lower blood glucose levels. For example, if a person weighs 200 pounds, a weight loss of 10-20 pounds can make a significant difference in managing prediabetes.
2. Regular Physical Activity
Exercise helps the body use insulin more effectively and lowers blood glucose levels. Aiming for at least 150 minutes of moderate-intensity exercise per week—such as brisk walking, swimming, or cycling—can help manage blood sugar levels and improve overall health.
3. A Healthy, Balanced Diet
A diet rich in whole grains, vegetables, lean proteins, and healthy fats can help stabilize blood glucose levels. Limiting refined carbohydrates, sugary foods, and processed snacks is essential for maintaining healthy glucose levels. Portion control and eating smaller, more frequent meals throughout the day can also help prevent blood sugar spikes.
4. Stress Management
Chronic stress can elevate blood sugar levels by triggering the release of stress hormones such as cortisol. Managing stress through relaxation techniques, mindfulness, yoga, or meditation can support better blood glucose control.
5. Adequate Sleep
Getting enough sleep—typically 7-9 hours per night—helps regulate insulin sensitivity. Poor sleep quality or insufficient sleep can negatively impact glucose metabolism, increasing the risk of prediabetes and type 2 diabetes.
Medical Interventions for Prediabetes
In addition to lifestyle modifications, healthcare professionals may recommend certain medications for individuals at high risk of developing type 2 diabetes. The most commonly prescribed medication for prediabetes is metformin, a drug that helps lower blood glucose levels and improve insulin sensitivity.
While lifestyle changes are usually the first line of defense, medications may be considered if an individual is at high risk of developing diabetes or if lifestyle changes alone are not enough to manage blood sugar levels.
Conclusion
Understanding when blood glucose levels fall into the prediabetic range is essential for preventing the progression to type 2 diabetes. Prediabetes is a serious health condition that requires attention and action. Regular blood glucose monitoring, combined with healthy lifestyle changes, can help individuals manage their blood sugar levels and significantly reduce their risk of developing type 2 diabetes.
By knowing the numbers that indicate prediabetes—fasting blood glucose between 100 and 125 mg/dL, 2-hour blood glucose between 140 and 199 mg/dL on an OGTT, or an A1c between 5.7% and 6.4%—individuals can take the necessary steps to safeguard their health. With early detection and intervention, prediabetes is a reversible condition, and lifestyle changes can help prevent the onset of diabetes and its associated complications.
Related topics:
How Does an Arm Glucose Monitor Work?